What is TMJ Disorder? Symptoms, Causes, and Treatment Options Explained
Have you ever experienced a clicking sound when chewing, or woken up with a sore jaw? You might be among the 10-15% of adults dealing with temporomandibular joint (TMJ) disorders. TMJ disorders affect the hinge connecting your jawbone to your skull, causing pain and dysfunction that can impact everything from eating to speaking.
Many people dismiss jaw discomfort as temporary stress or dental issues, but understanding TMJ is crucial for proper management. In this comprehensive guide, we’ll explore what TMJ disorder really is, identify its most common symptoms, uncover the underlying causes, and review both professional and at-home treatment options. Whether you’re seeking answers for your own symptoms or supporting someone with jaw pain, this article provides the essential knowledge you need.
Section 1: Understanding the Temporomandibular Joint
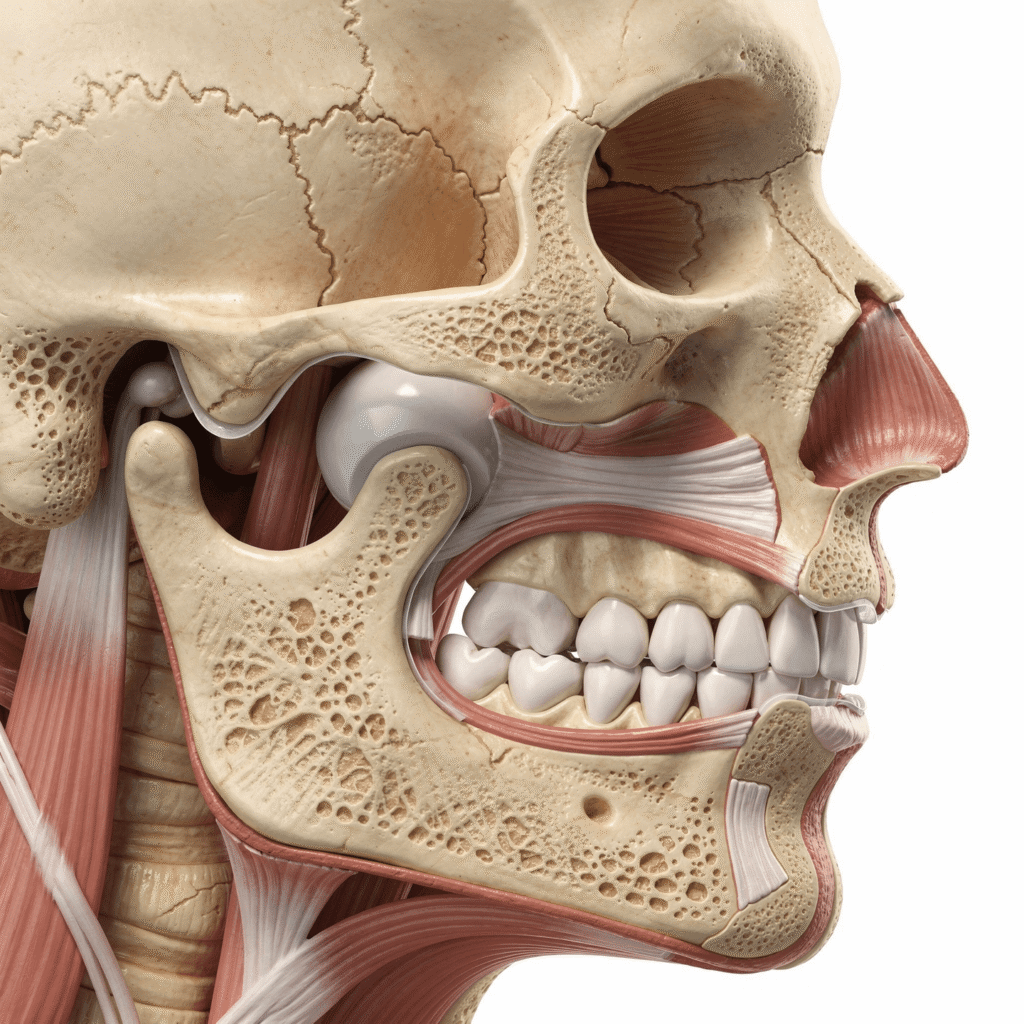
The temporomandibular joint (TMJ) is one of the most complex joints in your body. Located on each side of your face, just in front of your ears, these joints connect your lower jaw (mandible) to your skull (temporal bone).
Key Functions of the TMJ:
- Hinged Movement: Allows your jaw to open and close like a hinge
- Sliding Motion: Enables forward, backward, and side-to-side movements
- Shock Absorption: Contains a small disc that cushions the joint
- Coordination: Works with muscles and ligaments for synchronized movement
What Makes TMJ Unique:
Unlike most joints that either rotate or slide, the TMJ does both simultaneously. This dual-action capability lets you perform complex movements like chewing, speaking, and yawning. However, this complexity also makes the joint more susceptible to disorders.
TMJ vs. TMD: What’s the Difference?:
While people often say “TMJ” when referring to jaw problems, the correct medical term is Temporomandibular Disorder (TMD). TMJ refers specifically to the joint itself, while TMD describes disorders affecting the joint and surrounding muscles.
Section 2: Common Symptoms of TMJ Disorders
TMJ disorders can manifest in various ways. Here are the most common symptoms to watch for:
Primary Symptoms :
- Jaw Pain or Tenderness: Especially in the joint area, cheeks, or temples
- Clicking or Popping Sounds: When opening or closing your mouth
- Limited Jaw Movement: Difficulty opening wide or moving side to side
- Locking of the Jaw: Getting stuck in open or closed positions
Secondary Symptoms:
- Ear-related Issues: Ear pain, ringing (tinnitus), or feeling of fullness
- Headaches: Particularly temple or behind-the-eye headaches
- Facial Pain: Radiating discomfort across cheeks and forehead
- Tooth Sensitivity: Without dental issues present
- Neck and Shoulder Pain: Due to muscle tension
Symptoms During Specific Activities:
- While Eating: Pain when chewing, especially hard foods
- Morning Symptoms: Jaw stiffness or pain upon waking
- During Stress: Increased clenching and associated pain
- When Speaking: Discomfort during prolonged talking
Pro Tip: Keep a symptom diary for 1-2 weeks, noting when symptoms occur and their severity. This information can be invaluable for healthcare providers.
Section 3: Primary Causes and Risk Factors
Understanding what causes TMJ disorders helps in both treatment and prevention.
Mechanical Causes:
- Joint Damage: Arthritis, injury, or dislocation
- Disc Displacement: The cushioning disc slips out of position
- Muscle Issues: Overuse, strain, or spasm of jaw muscles
Common Triggers:
- Bruxism: Teeth grinding or clenching, often during sleep
- Trauma: Direct injury to jaw or whiplash
- Dental Issues: Malocclusion (bad bite) or recent dental work
- Stress: Leading to increased muscle tension
- Poor Posture: Especially forward head position
Risk Factors:
- Gender: Women are 2-3 times more likely to develop TMD
- Age: Most common between 20-40 years
- Medical Conditions: Arthritis, fibromyalgia, sleep apnea
- Lifestyle Factors: Gum chewing, nail biting, resting chin on hand
- Genetic Factors: Family history of TMJ disorders
Section 4: When to Seek Professional Help
While mild TMJ symptoms often improve with self-care, certain signs warrant professional evaluation.
Red Flags Requiring Immediate Attention :
- Sudden inability to open or close jaw
- Severe pain preventing eating or drinking
- Jaw locking in position
- Significant swelling in jaw area
- Fever accompanying jaw pain
When to Schedule a Non-Emergency Appointment
- Symptoms persisting beyond 2-3 weeks
- Progressive worsening of symptoms
- Pain interfering with daily activities
- Noticeable changes in bite alignment
- Failed response to at-home remedies
Healthcare Providers to Consult
- Dentist: First line for evaluation, especially if bruxism is suspected
- Primary Care Physician: For initial assessment and referral
- TMJ Specialist/Oral Surgeon: For complex cases
- Physical Therapist: For muscle-related issues
- Pain Management Specialist: For chronic pain cases
Section 5: Professional Treatment Options
Conservative Approaches (First Line) :
- Occlusal Splints/Night Guards: Custom-fitted oral appliances
- Physical Therapy: Jaw exercises, ultrasound, massage
- Medications:
- NSAIDs for inflammation
- Muscle relaxants for spasms
- Low-dose antidepressants for chronic pain
Moderate Interventions:
- Trigger Point Injections: For muscle knots
- Corticosteroid Injections: For joint inflammation
- Arthrocentesis: Joint fluid removal and flushing
- Transcutaneous Electrical Nerve Stimulation (TENS): Muscle relaxation
Surgical Options (Last Resort) :
- Arthroscopy: Minimally invasive joint examination and repair
- Open-Joint Surgery: For severe structural problems
- Joint Replacement: In extreme, debilitating cases
Important: Always start with the least invasive options. Most TMJ disorders improve with conservative treatment.
Section 6: At-Home Management Strategies
Immediate Relief Techniques
- Moist Heat Application: 15-20 minutes, 3-4 times daily
- Cold Packs: For acute inflammation (first 48 hours)
- Soft Diet: Avoid hard, chewy, or crunchy foods
- Jaw Rest: Limit talking, chewing, and yawning
Long-Term Management :
- Stress Reduction: Meditation, deep breathing, yoga
- Posture Correction: Ergonomic adjustments
- Awareness Training: Recognizing and stopping clenching
- Sleep Position: Back sleeping with proper pillow support
Recommended Exercises :
(Note: Detailed exercises covered in our separate article)
- Gentle stretching
- Range-of-motion exercises
- Resistance training (after acute phase)
Section 7: Prevention Tips
Daily Habits to Adopt
- Mindful Eating: Cut food into small pieces
- Avoid Extreme Jaw Movements: Limit wide yawning
- Proper Phone Use: Don’t cradle phone between ear and shoulder
- Regular Breaks: If you talk or chew frequently
Ergonomic Adjustments :
- Computer screen at eye level
- Supportive chair with proper back support
- Relaxed shoulder position
- Feet flat on floor
Stress Management Techniques :
- Regular exercise
- Adequate sleep (7-9 hours)
- Mindfulness practices
- Scheduled relaxation periods
Section 8: Frequently Asked Questions
Q1: Can TMJ disorder go away on its own?
A: Mild cases often improve with self-care within weeks. Chronic cases typically require some form of management.
Q2: Is TMJ disorder permanent?
A: Not necessarily. Many people achieve significant improvement or complete resolution with proper treatment.
Q3: Can stress really cause TMJ?
A: Stress doesn’t directly cause TMJ disorders but can exacerbate symptoms through increased muscle tension and clenching.
Q4: What’s the best sleeping position for TMJ?
A: Sleeping on your back with a supportive pillow is generally recommended to avoid jaw pressure.
Q5: How long does TMJ treatment take to work?
A: Conservative treatments often show improvement within 4-6 weeks, but complete resolution may take several months.
Q6: Can TMJ cause ear problems?
A: Yes, the TMJ is located close to the ear, and inflammation can cause ear pain, ringing, or fullness.
Q7: Should I use heat or ice for TMJ pain?
A: Use ice for acute pain/inflammation (first 48 hours), then switch to moist heat for muscle relaxation.
Q8: Can dentists treat TMJ disorders?
A: Many dentists are trained in TMJ management and can provide night guards, occlusal adjustments, and referrals.
Q9: Are there any exercises I should avoid?
A: Avoid forceful stretching, wide opening exercises during acute phases, or any movement causing pain.
Q10: When should I consider surgery?
A: Only after conservative treatments have failed, symptoms severely impact quality of life, and structural issues are confirmed.
TMJ disorders, while common and often uncomfortable, are manageable with the right approach. Understanding your symptoms and their potential causes is the first step toward effective treatment. Remember that most cases respond well to conservative measures like stress management, jaw exercises, and lifestyle adjustments.
If you suspect you have a TMJ disorder, start with gentle self-care strategies and monitor your symptoms. Don’t hesitate to seek professional guidance if pain persists or interferes with daily life. With proper care and patience, most individuals find significant relief and regain comfortable jaw function.
Next Steps: Consider exploring our detailed guide on TMJ exercises you can safely perform at home, or learn about dietary adjustments that can support jaw health.

