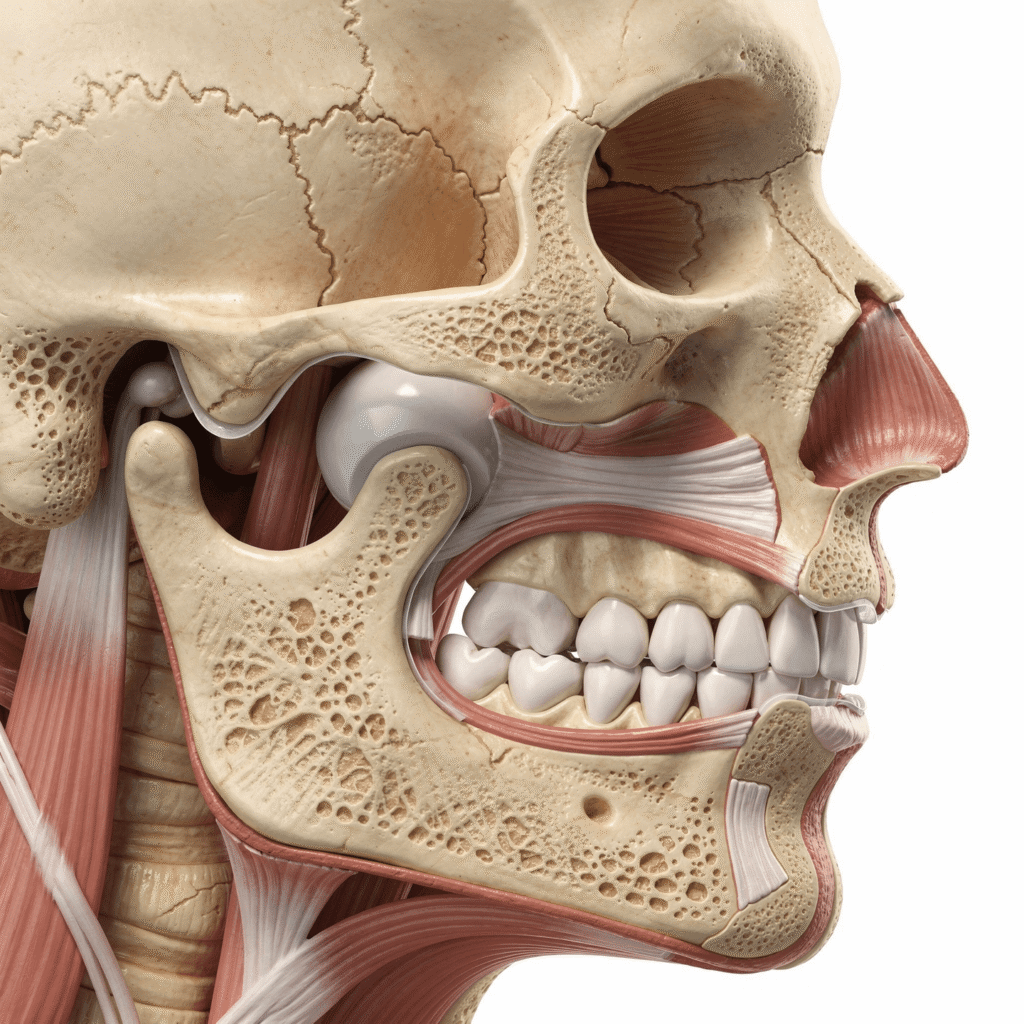
TMJ and Headaches. It starts as a faint tension behind your eyes, then spreads—temples throbbing, jaw aching, neck tightening until the pain becomes a single, unbearable experience. You’ve tried migraine medications, tension headache remedies, even jaw exercises, but relief is temporary at best. What if these aren’t separate conditions battling for attention, but different symptoms of the same underlying issue? The connection between TMJ disorders and chronic headaches is more than coincidence; it’s a physiological relationship that, when understood, opens doors to more effective, comprehensive relief.
The Overlooked Epidemic: When Headaches Are More Than “Just Headaches”
Medical research reveals a startling overlap: approximately 50-70% of TMJ sufferers also experience chronic headaches or migraines. Yet in clinical practice, these conditions are often treated in isolation—neurologists for the headaches, dentists for the jaw, physical therapists for the neck. This fragmented approach misses the crucial truth: your head, neck, and jaw form an integrated system where dysfunction in one area inevitably affects the others.
Consider Sarah’s experience (name changed for privacy): “For years, I saw a neurologist for migraines and a separate specialist for my jaw clicking. Neither asked about the other symptoms. It wasn’t until a physical therapist connected the dots that I realized my ‘migraine triggers’—stress, poor sleep, certain foods—were also my worst TMJ flare-up triggers.”
This dual suffering isn’t merely about having two separate pain conditions. It’s about a single dysfunctional system manifesting in multiple locations. Understanding this connection isn’t just academic—it’s the key to breaking cycles of pain that medications alone can’t address.
The Three Pathways: How TMJ Pain Travels to Your Head
Pathway 1: The Trigeminal Nerve Highway
Your trigeminal nerve—the largest cranial nerve—is the primary culprit in the TMJ-headache connection. This nerve has three branches that provide sensation to your entire face, teeth, jaw muscles, and parts of your meninges (the protective layers around your brain).
How it works: When your TMJ is irritated—whether from misalignment, inflammation, or muscle tension—it stimulates the trigeminal nerve. This nerve doesn’t distinguish well between different types of facial pain. The irritation can spread along the nerve pathways, manifesting as:
- Temple pain (temporal headache)
- Pain behind the eyes (often misdiagnosed as sinus headache)
- Forehead tension (tension-type headache)
- Even referred pain to the top or back of the head
Pathway 2: Muscle Referral Patterns
Your jaw muscles don’t work in isolation. The masseter (your main chewing muscle) and temporalis (temple muscle) have direct connections to muscles that control head and neck movement.
The cascade effect:
- TMJ dysfunction → jaw muscle overactivity
- Jaw muscle tension → compensatory neck muscle tension
- Neck muscle tension → suboccipital muscle strain
- Suboccipital strain → tension headaches at skull base
- Chronic tension → trigger points that refer pain to forehead/temples
This explains why many people with TMJ notice their headaches start at the base of their skull and travel forward—a classic tension headache pattern with a jaw-related origin.
Pathway 3: Central Sensitization
When pain persists for months or years, your nervous system can become “sensitized”—it starts overreacting to normal stimuli. This isn’t psychological; it’s a physiological change in how your brain processes pain signals.
For TMJ-headache sufferers: Initially, you might only get headaches during severe TMJ flare-ups. Over time, as central sensitization develops, milder jaw tension can trigger full-blown headaches. The threshold for pain activation lowers, creating a vicious cycle where each condition worsens the other.
Decoding Your Pain: Which Headache Type Do You Have?
Not all headaches from TMJ are created equal. Identifying your specific pattern guides more effective treatment:
Tension-Type Headaches from TMJ
Characteristics:
- Bilateral (both sides)
- Band-like pressure around head
- Often originates at skull base
- Worse as day progresses
- Related to jaw clenching episodes
TMJ Connection: Direct muscle tension referral from masseter and temporalis muscles.
Quick Test: Gently press on your jaw muscles while having a headache. If pressure increases head pain, you’re likely dealing with muscle-referred tension headaches.
Migraine-Like Headaches from TMJ
Characteristics:
- Often unilateral (one side)
- Throbbing/pulsating quality
- Light/sound sensitivity
- Possible aura (visual disturbances)
- Nausea sometimes present
TMJ Connection: Trigeminal nerve irritation triggering neurovascular changes similar to migraines.
Important Distinction: These are technically “migrainous headaches” rather than true migraines, but the experience and many treatments overlap.
Cervicogenic Headaches (Neck-Originating)
Characteristics:
- Starts in neck, radiates to head
- Limited neck mobility
- Pain with certain head movements
- Often one-sided
- May include shoulder/arm symptoms
TMJ Connection: Jaw dysfunction altering neck posture and muscle balance.
Cluster Headaches (Less Common but Possible)
Characteristics:
- Severe, explosive pain around one eye
- Occurs in “clusters” (weeks/months of daily attacks)
- Autonomic symptoms (tearing, nasal congestion)
- Extreme restlessness during attack
TMJ Connection: Emerging research suggests some cluster headaches may involve trigeminal-autonomic pathways that TMJ dysfunction could potentially influence.
The Diagnostic Dilemma: Are Your Headaches Caused by TMJ?
Ask yourself these questions:
- Timing Pattern: Do headaches typically follow or accompany jaw pain flare-ups?
- Location Correlation: Is your headache worst on the same side as your most painful TMJ?
- Trigger Overlap: Do headache and TMJ flare-ups share common triggers (stress, poor sleep, certain foods)?
- Manual Influence: Does gently massaging your jaw muscles affect headache intensity?
- Dental Connection: Have dental procedures or bite changes coincided with headache pattern changes?
- Positional Factors: Do certain head or jaw positions trigger both?
If you answer “yes” to three or more, TMJ likely contributes significantly to your headaches.
Professional Assessment Tools:
- Digital palpation: Practitioner checks for muscle tenderness in jaw, temples, neck
- Joint loading tests: Gentle pressure on TMJ reproduces headache symptoms
- Diagnostic anesthesia: Numbing specific areas temporarily relieves headache
- Imaging: MRI/CT to rule out other causes and assess joint condition
Dual-Action Relief: Strategies That Address Both TMJ and Headaches
Immediate Relief During an Attack
The 5-5-5 Protocol:
- 5 minutes of heat: Warm compress on jaw and neck muscles
- 5 minutes of gentle movement:
- Slow neck rotations (if not dizzy)
- Gentle jaw opening/closing
- Shoulder rolls
- 5 minutes of pressure point therapy:
- Masseter muscle: Press cheek while slowly opening mouth
- Temporal region: Circular massage at temples
- Suboccipital release: Base of skull pressure with head resting
Medication Considerations: While over-the-counter options can help, beware of medications that increase bruxism (like certain SSRIs) or rebound headaches with overuse.
Daily Prevention Strategies
Morning Routine (5 minutes):
- Cervical retraction exercises (chin tucks)
- Gentle jaw stretches
- Diaphragmatic breathing practice
Workday Integration (every 60 minutes):
- Posture check and reset
- 30-second jaw relaxation (teeth apart, lips together, tongue up)
- Shoulder and neck mobility breaks
Evening Wind-Down (15 minutes before bed):
- Progressive muscle relaxation starting at feet, ending at jaw
- Moist heat application to jaw and neck
- Mindfulness meditation focusing on releasing facial tension
Long-Term Management
Professional Interventions:
- Physical therapy addressing both cervical and TMJ components
- Occlusal splints (night guards) to reduce nocturnal clenching
- Trigger point injections for stubborn muscle knots
- Botox therapy for chronic muscle overactivity (when appropriate)
- Cognitive behavioral therapy for pain coping strategies
For comprehensive TMJ management approaches, explore our guide on TMJ Disorder Symptoms, Causes, and Treatment.
The Stress-Headache-Jaw Triangle: Breaking the Cycle
Stress doesn’t just cause headaches or worsen TMJ—it creates a self-perpetuating triangle:
Stress
↑ ↓
TMJ Pain ←→ Headaches
Breaking each link:
- Stress → TMJ: Mindfulness, breathing exercises, stress management
- TMJ → Headaches: Proper alignment, muscle balance, joint health
- Headaches → Stress: Pain coping strategies, medication management
- Stress → Headaches: Lifestyle modifications, trigger management
Effective stress-reduction techniques specifically for TMJ-headache sufferers:
- Diaphragmatic breathing with jaw relaxation cue
- Progressive muscle relaxation with extra focus on facial muscles
- Biofeedback training for jaw muscle awareness
- Guided imagery specifically for head and jaw tension release
Discover more stress-management strategies in our article TMJ and Stress: Breaking the Cycle of Jaw Tension.
When to Seek Specialized Help: Red Flags and Referrals
Urgent Evaluation Needed If:
- Sudden, severe headache unlike any previous
- Headache with fever, stiff neck, confusion
- Headache following head injury
- Neurological symptoms (weakness, vision changes, speech difficulties)
Specialist Referral Considerations:
Neurologist: For diagnosis of primary headache disorders, medication management
TMJ Specialist/Dentist: For bite assessment, oral appliances, joint treatment
Physical Therapist: For musculoskeletal components, exercise prescription
Pain Management: For interdisciplinary approach to chronic pain
Psychologist: For pain coping, stress management, sleep improvement
The Interdisciplinary Approach
Increasingly, headache and TMJ centers recognize the need for coordinated care. An ideal team might include:
- Neurologist ruling out other headache causes
- TMJ specialist addressing joint/dental factors
- Physical therapist optimizing musculoskeletal function
- Psychologist addressing pain coping and stress
FAQ: Your TMJ-Headache Questions Answered
Q1: Can treating my TMJ completely eliminate my headaches?
A: For headaches primarily caused by TMJ dysfunction, significant reduction or elimination is possible. For headaches with multiple contributing factors, TMJ treatment can substantially reduce frequency and severity even if not achieving 100% elimination.
Q2: How long until I see improvement in headaches after starting TMJ treatment?
A: Muscle-related tension headaches often show improvement within 2-4 weeks of consistent TMJ management. More complex headache patterns may take 2-3 months of combined therapies. Patience and consistency are key.
Q3: Are there specific medications that help both TMJ and headaches?
A: Some medications address both: muscle relaxants for tension components, certain antidepressants for pain modulation, and anti-inflammatories for joint inflammation. However, medication should be part of a comprehensive plan, not standalone treatment.
Q4: Can poor posture really cause both TMJ and headaches?
A: Absolutely. Forward head posture increases strain on both cervical spine and jaw muscles. Correcting posture can simultaneously reduce tension headaches and TMJ symptoms. Consider integrating postural exercises from our TMJ and Posture guide.
Q5: What’s the relationship between sleep, TMJ, and headaches?
A: This is a crucial triangle. Poor sleep increases pain sensitivity and muscle tension, worsening both TMJ and headaches. TMJ pain disrupts sleep quality. Headaches themselves interfere with sleep. Addressing sleep is often foundational to breaking this cycle.
Q6: Should I get imaging for my TMJ-related headaches?
A: If headaches are new, changing pattern, or accompanied by concerning symptoms, imaging (MRI/CT) helps rule out other causes. For chronic, stable TMJ-related headaches, imaging may be less urgent but can guide specific treatments.
Q7: Are there specific exercises to avoid with TMJ-headaches?
A: Avoid exercises that involve extreme jaw positions, heavy jaw loading, or neck hyperextension. High-impact activities that jar the head/jaw may also exacerbate symptoms during flare-ups.
Q8: Can children have TMJ-related headaches?
A: Yes, especially with increased screen time and device usage. Watch for complaints of jaw pain with headaches, increased clenching/grinding, or avoidance of chewy foods alongside headaches.
Creating Your Personalized Management Plan
Step 1: Tracking and Pattern Recognition
Maintain a 30-day diary tracking:
- Headache intensity/location/duration
- Jaw symptoms simultaneously
- Suspected triggers
- Interventions attempted and results
- Sleep quality and duration
Step 2: Conservative Interventions First
Begin with:
- Postural correction and ergonomic adjustments
- Stress management techniques
- Gentle exercises and stretches
- Dietary modifications (reduce inflammatory foods)
- Sleep optimization
Step 3: Professional Assessment
If conservative measures insufficient after 4-6 weeks:
- Comprehensive dental/TMJ evaluation
- Neurological assessment if indicated
- Physical therapy evaluation
- Consider multidisciplinary pain clinic referral
Step 4: Integration and Maintenance
Combine effective elements into sustainable daily routine:
- Morning: Prevention exercises
- Daytime: Posture/stress management
- Evening: Relaxation and preparation for restful sleep
- Ongoing: Professional support as needed
The Mindset Shift: From Sufferer to Manager
The journey with TMJ-related headaches involves a crucial psychological transition: from passive sufferer to active manager. This doesn’t mean the pain disappears, but rather that you develop tools, understanding, and resilience.
Remember:
- Progress isn’t linear—some days will be better than others
- Small consistent actions create cumulative change
- You’re not “just a headache sufferer”—you’re managing a complex physiological interplay
- Each strategy you learn and implement makes you more empowered
Your toolkit now includes:
- Understanding of the physiological connections
- Immediate relief strategies for acute episodes
- Daily practices for prevention
- Knowledge of when and how to seek professional help
- A framework for tracking and adjusting your approach
Conclusion: Reclaiming Your Days from Dual Pain
The connection between your jaw and your headaches isn’t a life sentence of double suffering—it’s a map showing where interventions can have multiplied effects. Treating your TMJ doesn’t just help your jaw; it can quiet the storm in your head. Addressing your headaches doesn’t just clear your thinking; it can relax your clenched jaw.
Start today by simply noticing: when a headache begins, check in with your jaw. Is it tight? Are you clenching? That moment of awareness is the first step toward interruption. Tomorrow, try one new strategy—perhaps the 5-5-5 protocol during an early headache, or a posture check every hour.
Healing happens in layers, not leaps. Each day you apply understanding and take action, you’re not just reducing today’s pain—you’re rewiring patterns that have taken years to develop. Your head and jaw have been communicating their distress; now you’re learning their language and, most importantly, how to respond with compassion and effectiveness.
For more resources on comprehensive TMJ management, explore our full library at NaturalWellness30.
Medical Disclaimer: This article provides educational information about the potential connection between TMJ disorders and headaches. It is not medical advice. Headaches can have serious underlying causes. Always consult with qualified healthcare professionals for proper diagnosis and treatment. Never disregard professional medical advice or delay seeking it because of information in this article.