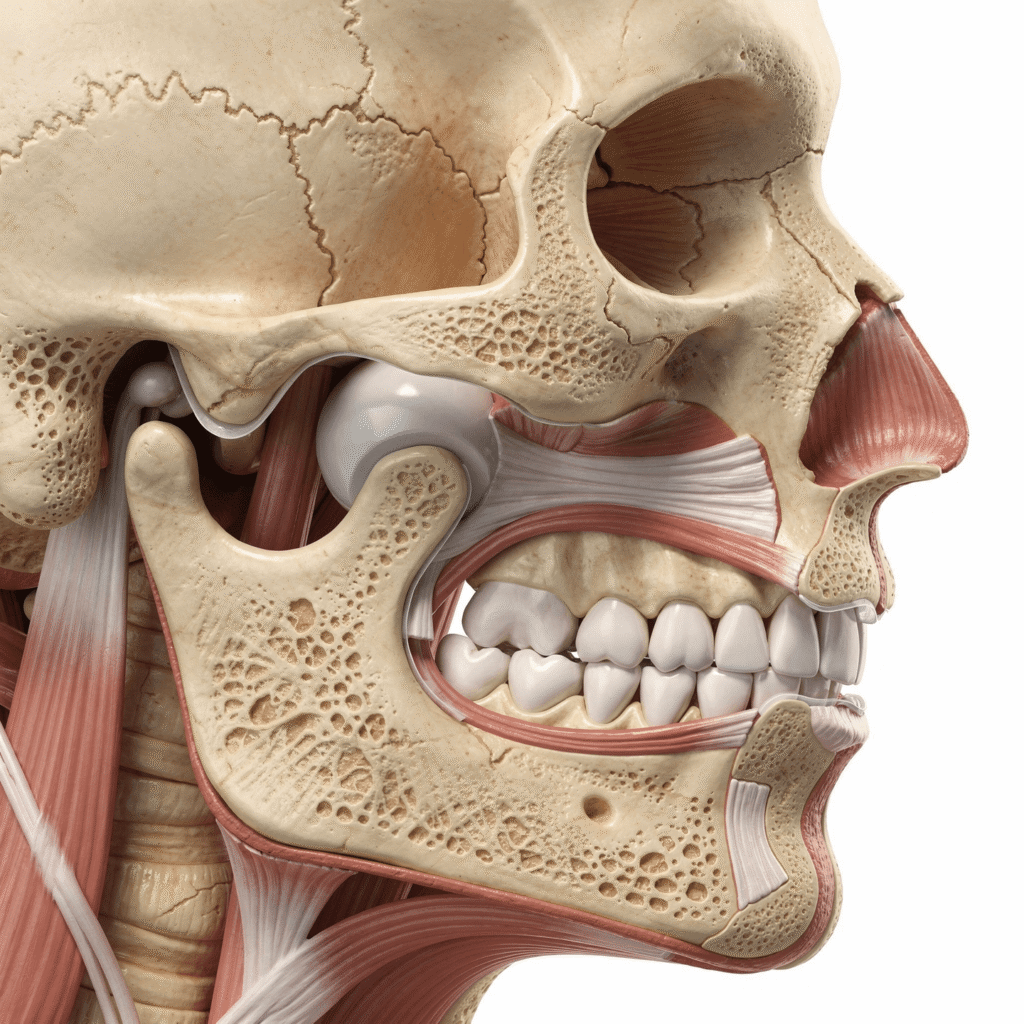
TMJ and Sleep. Have you ever found yourself staring at the ceiling at 3 AM, your jaw throbbing with a dull ache that seems to pulse with every heartbeat? You’re not alone. For millions, the bedroom—a place meant for rest—becomes a battleground where TMJ disorders wage war against sleep. But what if you could break this exhausting cycle?
The Vicious Cycle: How TMJ Pain and Poor Sleep Feed Each Other
It starts innocently enough. A slight tension in your jaw after a stressful day. A faint clicking when you chew dinner. But as night falls, the symptoms amplify. That tension becomes a clenched jaw grinding against itself. The clicking gives way to stiffness that makes yawning painful. Soon, you’re trapped in what sleep specialists call the “pain-insomnia-pain cycle.”
Here’s how it works: TMJ pain activates your sympathetic nervous system—your body’s “fight or flight” response. This system releases stress hormones like cortisol that make falling asleep difficult. The less you sleep, the lower your pain threshold drops. Studies show that sleep deprivation can increase pain sensitivity by up to 200%. The result? Your normal TMJ discomfort feels excruciating, which keeps you awake even more.
But there’s hope. Understanding this connection is the first step toward breaking free. In this comprehensive guide, we’ll explore practical, science-backed strategies to help you achieve the restful sleep you deserve, starting tonight.
The TMJ-Sleep Connection: Why Your Jaw Keeps You Awake
The Science Behind the Sleepless Nights
Your temporomandibular joint is one of the most complex in your body. It’s a sliding hinge that combines hinge and gliding motions, controlled by an intricate network of muscles, ligaments, and nerves. When this system malfunctions—whether from misalignment, arthritis, injury, or chronic clenching—it doesn’t just affect chewing.
The trigeminal nerve, responsible for sensation in your face and motor functions like biting, has extensive connections throughout your nervous system. When irritated by TMJ dysfunction, it can:
- Trigger muscle spasms that prevent relaxation
- Cause referred pain to your temples, neck, and even shoulders
- Activate stress responses that interfere with sleep onset
- Exacerbate or mimic conditions like tension headaches
Bruxism: The Nighttime Saboteur
Approximately 70% of TMJ-related sleep issues involve bruxism—unconscious teeth grinding or clenching during sleep. While occasional bruxism is normal, chronic grinders can exert up to 250 pounds of force on their teeth—six times more than during normal chewing.
This isn’t just about dental damage. The constant muscle activity:
- Prevents your jaw muscles from entering the restorative relaxation phase
- Maintains low-level brain activity that interferes with deep sleep stages
- Creates micro-arousals (brief awakenings) throughout the night
- Leads to morning symptoms: jaw soreness, headaches, tooth sensitivity
The good news? With targeted interventions, this cycle is breakable. The strategies below have helped thousands reclaim their sleep.
3 Sleep Positions That Reduce TMJ Pain (And 2 to Avoid)
Your sleeping position dramatically impacts jaw alignment and muscle tension. Making simple adjustments can provide immediate relief.
✅ Best Position #1: Supported Side Sleeping
Why it works: Side sleeping naturally opens the airway slightly, reducing the likelihood of mouth breathing (which can dry oral tissues and increase grinding). With proper pillow support, it maintains spinal alignment.
How to optimize it:
- Choose a pillow that fills the space between your ear and shoulder completely
- Place a small, firm pillow between your knees to prevent spinal rotation
- Consider a contoured pillow with extra support for the neck
- For TMJ-specific relief: Add a thin pillow or rolled towel under the side of your jaw for gentle support
Ideal pillow: Medium-firm memory foam or buckwheat hull with cervical contour
✅ Best Position #2: Semi-Reclined Back Sleeping
Why it works: Elevating your upper body reduces fluid accumulation around the jaw joint, decreases acid reflux (which can worsen bruxism), and promotes nasal breathing.
How to optimize it:
- Use a wedge pillow (typically 30-45 degree angle) or adjustable bed
- Ensure your neck maintains its natural curve—don’t let it bend forward
- Place a small pillow under your knees to reduce lower back strain
- TMJ tip: Practice relaxing your jaw completely before sleep in this position
Ideal pillow: Therapeutic wedge pillow or adjustable bed frame
✅ Best Position #3: Modified Fetal Position
Why it works: This curled position can reduce muscle tension throughout the posterior chain, but requires careful modification to prevent jaw compression.
How to optimize it:
- Don’t curl too tightly—maintain some space between chin and chest
- Place a body pillow to hug, which prevents shoulder roll-forward
- Ensure your head pillow supports both head and upper shoulder
- Critical adjustment: Keep your bottom arm extended slightly forward, not trapped under your body
Ideal pillow: Full-body pillow combined with supportive head pillow
❌ Positions to Avoid:
Stomach Sleeping: The worst position for TMJ sufferers. It forces neck rotation (often 90 degrees) and creates uneven pressure on one side of the jaw. This can exacerbate joint inflammation and muscle imbalance.
Flat Back Sleeping Without Support: While back sleeping itself isn’t bad, lying completely flat can encourage mouth opening and jaw dropping backward, straining the temporomandibular joint.
Your Pre-Sleep TMJ Relief Routine (30-Minute Protocol)
Consistency transforms occasional relief into lasting change. This 30-minute routine, when performed nightly, can significantly reduce nighttime symptoms within 2-3 weeks.
Minute 0-5: Warm-Up Phase
Heat Therapy Application
- Use a moist warm compress (not dry heat) on both sides of your jaw
- Temperature should be warm but comfortable (not hot)
- Apply for 5 minutes to increase blood flow and relax muscles
- Alternative: Take a warm shower, allowing water to flow over neck and jaw
Minute 5-15: Gentle Movement Phase
Three Targeted Jaw Stretches
- Resisted Mouth Opening
- Place thumb under chin, index finger on chin
- Gently press as you slowly open mouth against resistance
- Hold slight stretch at comfortable opening for 5 seconds
- Repeat 5 times
- Side-to-Side Glide
- Place tongue on roof of mouth
- Slowly move jaw side to side without opening mouth
- Keep movements small and controlled
- 10 repetitions each side
- Chin Tucks
- Sit or stand with good posture
- Gently draw chin straight back (creating “double chin”)
- Hold for 5 seconds, release
- 10 repetitions
For a more comprehensive exercise guide, explore our 10 Simple TMJ Exercises You Can Do at Home Today.
Minute 15-20: Nervous System Calming
4-7-8 Breathing Technique
- Sit comfortably with back straight
- Exhale completely through mouth
- Inhale quietly through nose for 4 seconds
- Hold breath for 7 seconds
- Exhale completely through mouth for 8 seconds
- Repeat this cycle 4 times
Why it works: This breathing pattern activates the parasympathetic nervous system—your body’s “rest and digest” mode—counteracting the stress response that fuels bruxism.
Minute 20-25: Muscle Release
Neck and Shoulder Tension Relief
- Shoulder Rolls: 10 forward, 10 backward (slow and deliberate)
- Neck Side Stretch: Gently pull head toward shoulder until mild stretch
- Scalp Release: Using fingertips, make small circles at temples and base of skull
Minute 25-30: Progressive Relaxation
Body Scan Technique
- Lie in your prepared sleeping position
- Starting at your feet, consciously relax each body part
- Pay special attention to jaw, tongue, forehead, and shoulders
- Mentally repeat “relax” as you exhale from each area
- Finish with 30 seconds of focused jaw relaxation: teeth slightly apart, lips together, tongue resting on roof of mouth
Choosing the Right Pillow: TMJ Edition
The wrong pillow can undo all your daytime efforts. Here’s what to look for:
Material Matters: Memory Foam vs. Buckwheat vs. Latex
| Material | Pros for TMJ | Cons | Best For |
|---|---|---|---|
| Memory Foam | Contours to neck shape, reduces pressure points | Can retain heat, may have odor initially | Side sleepers, those with arthritis |
| Buckwheat Hull | Fully adjustable loft, excellent support, cool | Heavy, rustling noise, firm feel | Combination sleepers, hot sleepers |
| Latex | Supportive yet responsive, naturally cooling, durable | Less contouring, heavier, higher cost | Back sleepers, allergy sufferers |
| Down/Feather | Soft, moldable, traditional comfort | Lacks support, can flatten over time | Those who prefer very soft surfaces |
Key Features for TMJ Sufferers
- Loft/Height: Should match your shoulder width when side sleeping
- Narrow shoulders: 3-4 inches
- Average shoulders: 4-5 inches
- Broad shoulders: 5-6 inches
- Contour Design: Look for cervical support with a deeper depression for the head and raised edges for neck support
- Hypoallergenic: Important if you have allergies that might cause mouth breathing
- Washability: Clean pillow = reduced allergens = better nasal breathing
When to Replace Your Pillow
- Memory foam: Every 2-3 years
- Latex: 3-4 years
- Buckwheat: Refresh hulls annually, replace entirely every 5 years
- Down: Every 2 years with professional cleaning
Quick test: Fold your pillow in half. If it doesn’t spring back immediately, it’s time for replacement.
Night Guards and Splints: What You Need to Know
Understanding Your Options
Over-the-Counter (OTC) Night Guards:
- Price: $20-$100
- Pros: Immediately available, affordable
- Cons: One-size-fits-all often fits poorly, can worsen misalignment, may increase clenching
- Best for: Temporary use, diagnostic tool to see if grinding decreases
Dentist-Made Custom Night Guards:
- Price: $300-$800 (rarely covered by insurance for TMJ)
- Pros: Perfect fit, designed for your specific bite, durable materials
- Cons: Cost, requires dental visits, adjustment period
- Best for: Chronic bruxism, severe TMJ symptoms, long-term use
Stabilization Splints (Orthotics):
- Price: $1,000-$3,000
- Pros: Actually reposition jaw, treat underlying dysfunction
- Cons: Very expensive, requires specialist, lengthy adjustment
- Best for: Significant TMJ dysfunction with documented malocclusion
How They Actually Work
Contrary to popular belief, night guards don’t just “cushion” your teeth. Their primary mechanisms:
- Creating proprioceptive awareness: The foreign object in your mouth increases awareness of jaw position
- Reducing muscle activity: Studies show properly fitted guards can reduce nocturnal muscle activity by 50-70%
- Preventing dental damage: A secondary but important benefit
- Equalizing pressure: Distributes forces across all teeth rather than specific points
Important Considerations
- The Adaptation Period: Most people experience increased salivation and slight discomfort for 1-2 weeks
- Cleaning is Crucial: Use non-abrasive cleaners to prevent bacterial growth
- Regular Check-ups: Even custom devices need occasional adjustment
- Not a Cure: Address underlying causes (stress, posture, airway issues) alongside device use
Medical Disclaimer: Night guards are medical devices. Consult with a dental professional to determine if one is appropriate for your specific condition. Incorrect use can worsen TMJ symptoms.
When Poor Sleep Isn’t “Just TMJ”: Red Flags
While TMJ disorders commonly disrupt sleep, sometimes sleep disturbances indicate more serious conditions that require professional evaluation.
Signs You Might Need a Sleep Study:
- Loud, chronic snoring interrupted by gasping or choking sounds
- Excessive daytime sleepiness despite adequate time in bed
- Witnessed apneas (someone sees you stop breathing during sleep)
- Morning headaches that differ from TMJ-related temple pain
- Cognitive issues: Memory problems, difficulty concentrating
- High blood pressure that’s difficult to control
The TMJ-Sleep Apnea Connection
Recent research reveals a bidirectional relationship:
- Sleep apnea → chronic mouth breathing → altered jaw development/position → TMJ disorders
- TMJ pain → poor sleep quality → increased inflammation → worsened sleep apnea
If you suspect overlap, a polysomnogram (sleep study) can diagnose sleep apnea. Treatment (often CPAP or oral appliance therapy) might significantly improve both conditions.
When to Seek Professional Help
Consult a TMJ specialist or dentist if:
- Pain prevents falling or staying asleep multiple nights weekly
- You experience locking or catching of the jaw
- Symptoms persist despite 4-6 weeks of consistent self-care
- Pain radiates to ears, neck, or causes headaches
Consult a sleep specialist if:
- You snore loudly or gasp during sleep
- Daytime fatigue affects work or driving safety
- You need caffeine to function
- Self-help strategies provide no improvement after 2 months
Frequently Asked Questions (FAQ)
Q1: Can TMJ disorder cause sleep apnea?
A: While TMJ doesn’t directly cause obstructive sleep apnea, they frequently coexist. Both conditions share risk factors like retrognathia (recessed jaw), mouth breathing, and inflammation. Treating one often improves the other.
Q2: Why does my TMJ pain get worse at night?
A: Three primary reasons: 1) Cortisol (natural anti-inflammatory) drops at night, 2) Lack of daytime distractions makes pain more noticeable, 3) Unconscious bruxism during sleep creates sustained muscle activity without rest periods.
Q3: What’s the best sleeping position for TMJ and shoulder pain?
A: Modified side sleeping with a body pillow offers the best compromise. Hug the body pillow to prevent shoulder roll-forward, and ensure your head pillow adequately supports both head and neck alignment.
Q4: How can I stop clenching my jaw in my sleep?
A: Daytime awareness is key. Set hourly reminders to check jaw position (teeth apart, lips together, tongue on roof of mouth). Evening relaxation routines and possibly a night guard can reduce nocturnal clenching.
Q5: Can a new pillow really help TMJ pain?
A: Yes, significantly. An improper pillow creates neck misalignment that strains jaw muscles all night. The right pillow supports cervical curvature, reducing strain on the temporomandibular joint complex.
Q6: Are there specific foods that make TMJ sleep issues worse?
A: Yes. Avoid hard, chewy, or crunchy foods after 6 PM. Also limit caffeine after noon, alcohol before bed (it fragments sleep), and high-sugar foods that can increase inflammation.
Q7: How long before I see improvement in my sleep with TMJ treatments?
A: Self-care strategies often show some improvement within 1-2 weeks. Significant, consistent improvement typically takes 4-8 weeks of diligent practice. Professional treatments vary based on type and individual response.
Q8: Is it safe to take sleep aids if I have TMJ?
A: Some over-the-counter sleep aids can increase bruxism. Prescription medications vary in their effects. Always consult both your dentist/TMJ specialist and physician before combining sleep medications with TMJ treatment.
Conclusion: Reclaiming Your Rest Starts Tonight
The journey from sleepless nights to restorative rest begins with understanding the intimate dance between your jaw and your sleep. TMJ disorders don’t have to sentence you to chronic fatigue and pain. By implementing the strategies in this guide—from optimizing your sleep position to establishing a consistent pre-sleep routine—you’re taking proactive steps toward breaking the pain-insomnia cycle.
Remember: Consistency beats perfection. Start with one change—perhaps the 30-minute pre-sleep routine or a pillow upgrade—and build from there. Your body’s healing processes work most effectively during deep sleep, so every improvement in sleep quality accelerates your TMJ recovery.
Ready to take the next step? Download our free “7-Day TMJ & Sleep Reset Guide”—a daily email program that walks you through evidence-based strategies to improve both jaw health and sleep quality. You’ll receive daily exercises, mindfulness practices, and tracking tools to monitor your progress.
Sweet dreams and pain-free mornings are closer than you think. Your journey to better sleep starts with your next breath.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended as medical advice. Always consult with qualified healthcare professionals for diagnosis and treatment of TMJ disorders or sleep conditions. Individual responses to treatments vary, and what works for one person may not work for another.