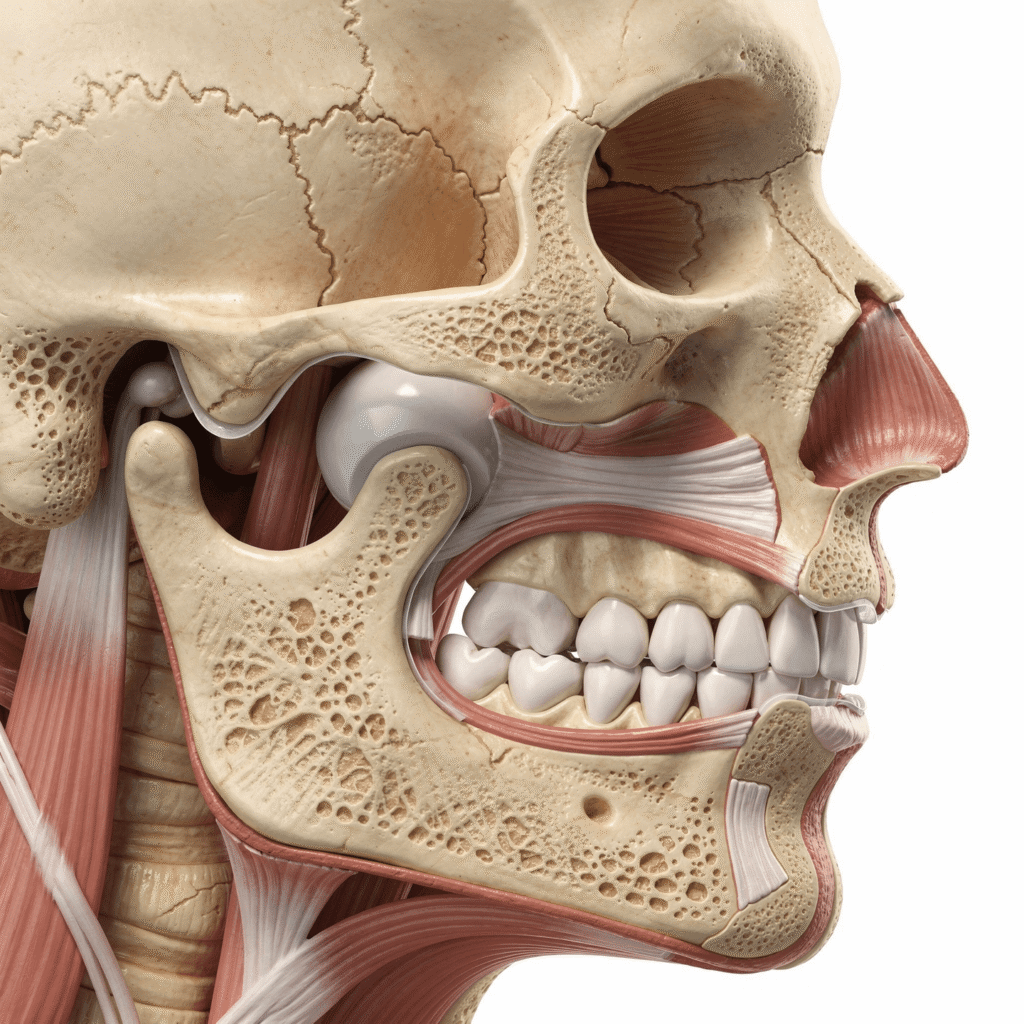
When to See a Doctor for TMJ Pain. You’ve tried the home remedies. You’ve done the jaw exercises. You’ve even tried sleeping on your back with the perfect pillow. But that jaw pain just won’t go away. Now you’re left wondering: Is this serious enough to see a doctor?
It’s a common question among TMJ sufferers. The temporomandibular joint is complex, and knowing when professional help is needed can be confusing. Some cases resolve with self-care, while others require medical intervention to prevent permanent damage.
In this guide, you’ll learn the 7 clear signs that indicate it’s time to seek professional help, what to expect during a TMJ evaluation, and how to choose the right healthcare provider for your specific symptoms. No more guessing – you’ll know exactly when to make that appointment.
Section 1: Understanding TMJ – When Self-Care Is Enough
Before diving into when to see a doctor, it helps to understand which TMJ symptoms often respond well to self-care.
Mild TMJ Symptoms That May Improve with Home Care:
- ✅ Occasional jaw tenderness after stressful days
- ✅ Mild clicking without pain
- ✅ Temporary discomfort after eating chewy foods
- ✅ Slight muscle tension that relaxes with warm compresses
- ✅ Occasional headaches related to jaw tension
Self-Care Strategies to Try First:
- Soft food diet for 1-2 weeks
- Warm compresses on the jaw area (15-20 minutes, 2-3x daily)
- Gentle jaw exercises (no forcing!)
- Stress reduction techniques (deep breathing, meditation)
- Awareness training – noticing and releasing daytime clenching
- Sleep position optimization (back sleeping with proper pillow support)
- Over-the-counter anti-inflammatories (ibuprofen, as directed)
If these strategies bring significant relief within 2-3 weeks, you may not need professional care – yet. But if symptoms persist or worsen, read on.
Section 2: Sign #1 – Persistent Pain That Won’t Go Away
What to Look For:
- Pain lasting more than 3-4 weeks despite self-care
- Pain that’s consistent (daily, not occasional)
- Discomfort that interferes with eating, speaking, or sleeping
Why This Matters:
Chronic pain changes how your nervous system processes signals. What starts as muscle tension can become centralized pain – meaning your brain becomes “stuck” in pain mode even after the original cause is gone.
When to Seek Help:
If you’ve tried self-care consistently for 3-4 weeks and your pain level hasn’t dropped by at least 50%, it’s time for a professional evaluation.
What a Doctor Will Look For:
- Underlying causes you might have missed
- Whether pain is muscular, joint-related, or both
- Signs of inflammation that need medical treatment
Section 3: Sign #2 – Jaw Locking (Open or Closed)
What to Look For:
- Open lock: Your mouth gets stuck in an open position and you can’t close it
- Closed lock: You can’t open your mouth wide enough to eat or speak properly
- Intermittent locking: Your jaw locks occasionally but then releases
Types of Locking:
| Type | Description | Urgency |
|---|---|---|
| Open lock | Mouth stuck open | EMERGENCY – seek care immediately |
| Closed lock | Can’t open mouth fully | URGENT – see specialist within days |
| Intermittent locking | Locks but releases | Schedule appointment soon |
Why This Happens:
The articular disc (small cushion between your jaw joint and skull) may have slipped out of place. In some cases, it’s displaced but the jaw still moves; in others, it completely blocks movement.
When to Seek Help:
- Immediately if your jaw locks open (go to ER or urgent care)
- Within 1-3 days if you can’t open your mouth enough to eat
- Within 1-2 weeks for intermittent locking
What a Doctor Will Do:
- Manual manipulation to reposition the disc (in some cases)
- Imaging to see the disc position (MRI)
- Referral to oral surgeon if severe
Section 4: Sign #3 – Severe or Worsening Headaches
What to Look For:
- Morning headaches that improve as the day goes on
- Temple headaches that feel like tension or pressure
- Migraine-like symptoms triggered by jaw use
- Headaches accompanied by jaw pain or clicking
The TMJ-Headache Connection:
The trigeminal nerve (the main nerve for your jaw) also supplies sensation to much of your head. When your jaw muscles are tense or your joint is inflamed, this nerve sends pain signals that your brain interprets as headaches.
Statistics:
- 70-85% of TMJ patients report frequent headaches
- TMJ treatment reduces headache frequency by 60-80% in many cases
- Morning headaches are 3x more common in people with sleep bruxism
When to Seek Help:
- Headaches occur 3+ times per week
- Over-the-counter pain relievers don’t help
- Headaches are getting worse over time
- You’re missing work or activities due to headache pain
Section 5: Sign #4 – Tooth Damage from Grinding
What to Look For:
- Flattened teeth – your teeth look shorter or worn down
- Chipped or cracked teeth – especially molars
- Worn enamel – teeth look shiny or transparent at edges
- Broken fillings or dental work – crowns, bridges, veneers damaged
- Tooth sensitivity – from exposed dentin
Why This Is Serious:
Once enamel is worn away, it doesn’t grow back. Severe tooth damage can lead to:
- Root canals
- Tooth loss
- Expensive dental reconstruction
- Chronic tooth sensitivity
The Grinding-Sleep Connection:
Most grinding happens during sleep, often without your awareness. You might wake with sore jaw muscles but not realize you’re causing permanent tooth damage every night.
When to Seek Help:
- You notice any of the above signs of tooth wear
- Your dentist mentions wear patterns during checkups
- You’ve already broken dental work from grinding
- Your partner says you grind your teeth at night
What a Doctor/Dentist Will Do:
- Assess the extent of tooth damage
- Recommend a night guard (custom-fitted)
- Possibly refer to a TMJ specialist for underlying causes
Section 6: Sign #5 – Ear Symptoms Without Infection
What to Look For:
- Ear pain without signs of infection (no fever, no fluid)
- Ringing in the ears (tinnitus) that comes and goes
- Fullness or pressure in one or both ears
- Dizziness or vertigo related to jaw movement
- Itchy ears with no visible cause
Why This Happens:
The TMJ sits directly in front of the ear canal. When inflamed, it can:
- Press on ear structures
- Irritate shared nerves
- Cause muscle tension that affects eustachian tube function
Common Misdiagnosis:
Many TMJ patients see multiple doctors for “ear infections” that don’t exist. They’re treated with antibiotics (which don’t work) while the real cause – TMJ – goes untreated.
When to See a Doctor:
- You’ve seen an ENT and they found no ear infection
- Ear symptoms worsen with jaw movement (chewing, talking)
- Ear pain is accompanied by other TMJ symptoms (clicking, jaw pain)
- You have tinnitus that varies with jaw position
Which Doctor to See:
Start with your primary care physician or an ENT to rule out actual ear disease. If they find nothing, ask for a TMJ referral.
Section 7: Sign #6 – Facial Swelling or Changes
What to Look For:
- Visible swelling in front of the ear or along the jawline
- Asymmetry – one side of your face looks different
- Hard lumps or nodules near the joint
- Warmth or redness over the TMJ area
Why This Is Urgent:
Swelling can indicate:
- Infection in the joint (septic arthritis)
- Inflammatory arthritis flare-up (rheumatoid, psoriatic)
- Cyst or tumor in rare cases
- Acute inflammation needing immediate treatment
When to Seek Help:
- IMMEDIATELY (go to ER or urgent care) if:
- Swelling is sudden and severe
- You have fever with joint swelling
- Swelling is spreading or red and hot
- You have difficulty breathing or swallowing
- Within 1-2 days if:
- Mild swelling that doesn’t improve
- You notice a lump or bump
- Swelling recurs periodically
What a Doctor Will Do:
- Examine the swelling
- Possibly order imaging (MRI, CT scan)
- Check for infection or inflammatory conditions
- Refer to appropriate specialist
Section 8: Sign #7 – TMJ Symptoms Affecting Daily Life
What to Look For:
- Difficulty eating – avoiding certain foods, eating less
- Trouble speaking – jaw fatigue during conversations
- Sleep disruption – pain wakes you up or prevents sleep
- Social avoidance – not going out because of pain or eating difficulties
- Mood changes – irritability, anxiety, depression related to pain
- Work impact – missing work or reduced productivity
Why Quality of Life Matters:
Pain isn’t just about physical sensation – it affects every aspect of your life. When TMJ symptoms start interfering with daily activities, it’s a clear sign that professional help is needed.
The Pain-Sleep-Stress Cycle:
text
TMJ Pain → Poor Sleep → More Stress → Worse Pain → Further Sleep Disruption → Quality of Life Declines
Professional treatment can help break this cycle.
When to Seek Help:
- You’ve changed your diet significantly due to pain
- You dread meals or social events involving food
- You’re losing sleep regularly
- You feel hopeless about your condition improving
- Pain affects your work performance
Section 9: Types of Healthcare Providers for TMJ
Not all providers are created equal. Here’s who does what:
1. General Dentist
- Best for: Initial evaluation, ruling out dental causes
- Can provide: Night guards, basic TMJ assessment
- Limitations: May not have specialized TMJ training
- When to see: First stop if you’re unsure where to go
2. Orofacial Pain Specialist
- Best for: Comprehensive TMJ diagnosis and treatment
- Can provide: Advanced treatment plans, splint therapy, medication management
- Training: 2+ years post-dental school specializing in pain
- When to see: Your primary choice for TMJ care
3. Oral and Maxillofacial Surgeon
- Best for: Surgical interventions when conservative care fails
- Can provide: Arthroscopy, joint surgery, trauma repair
- Training: Surgical specialty
- When to see: Only after conservative treatment has been tried
4. Physical Therapist (specializing in TMJ)
- Best for: Muscle-related TMJ issues, posture correction
- Can provide: Exercises, manual therapy, ultrasound, dry needling
- Training: Specialized continuing education in craniofacial therapy
- When to see: For muscle tension, posture issues, post-surgical rehab
5. Primary Care Physician
- Best for: Ruling out other conditions, medication management
- Can provide: Referrals to specialists, pain medications
- Limitations: Limited TMJ-specific training
- When to see: If you need a referral for insurance, or have other health concerns
6. Rheumatologist
- Best for: TMJ related to arthritis (rheumatoid, psoriatic, etc.)
- Can provide: Disease-modifying treatments for inflammatory conditions
- Training: Arthritis and autoimmune disease specialist
- When to see: If you have known arthritis or autoimmune disease
7. Psychologist/Psychiatrist
- Best for: Stress-related TMJ, pain coping strategies
- Can provide: Cognitive behavioral therapy, biofeedback, stress management
- Training: Mental health professional with pain specialization
- When to see: If stress and anxiety significantly worsen your symptoms
Section 10: What to Expect During a TMJ Evaluation
Knowing what happens at a TMJ appointment can reduce anxiety and help you prepare.
Before Your Appointment:
- Track your symptoms for 1-2 weeks (pain levels, triggers, patterns)
- List your questions (write them down!)
- Gather records: Previous dental X-rays, medical history, medications
- Note what helps and what makes it worse
During the Evaluation:
A comprehensive TMJ exam typically includes:
1. Health History Review
- Medical and dental history
- Symptom timeline
- Previous treatments and results
- Medications and supplements
2. Physical Examination
- Palpation: Feeling jaw muscles and joints for tenderness
- Range of motion: Measuring how wide you can open
- Joint sounds: Listening for clicking, popping, crepitus
- Bite analysis: How your teeth come together
- Posture assessment: Head, neck, and shoulder position
3. Possible Imaging
- Panoramic X-ray: General view of teeth and jaws
- CBCT (3D X-ray): Detailed view of bone structure
- MRI: To see the disc and soft tissues
- Arthroscopy: Camera in the joint (rare for initial visit)
4. Diagnosis Discussion
- What type of TMJ disorder you have (muscular, joint, or both)
- Contributing factors identified
- Treatment options presented
After the Appointment:
You should leave with:
- A clear diagnosis (or next steps for diagnosis)
- Treatment options explained (with pros and cons)
- A recommended treatment plan
- Understanding of costs and timeline
Section 11: Questions to Ask Your Provider
Print this list and take it to your appointment:
About Diagnosis:
- What type of TMJ disorder do I have?
- Is this muscular, joint-related, or both?
- What caused my condition?
- Do I need any imaging tests? Why?
About Treatment Options:
- What are my treatment options?
- What do you recommend starting with?
- What are the pros and cons of each option?
- How long will treatment take?
- What results can I realistically expect?
About Self-Care:
- What can I do at home to help?
- Are there exercises I should do (or avoid)?
- Should I change my diet?
- What about stress management?
About Prognosis:
- Will this ever go away completely?
- What happens if I don’t treat it?
- How often will I need follow-up appointments?
- When should I come back if things get worse?
Practical Questions:
- Is this covered by my insurance?
- What are the costs?
- Do I need a referral from my primary doctor?
Section 12: Red Flags – When to Go to the Emergency Room
Go to the ER or Urgent Care immediately if you experience:
🚨 TRUE EMERGENCIES:
- Sudden inability to open or close your jaw (locked open)
- Severe swelling with fever (possible infection)
- Difficulty breathing or swallowing
- Sudden, severe pain that comes on quickly
- Numbness or tingling in your face (possible nerve involvement)
- Trauma – recent injury to the jaw or face
URGENT (See doctor within 24-48 hours):
- Jaw locked closed (can’t open enough to eat)
- Severe pain uncontrolled by OTC medication
- Spreading redness or warmth over the joint
- New neurological symptoms (facial droop, weakness)
FAQ (Frequently Asked Questions)
1. “Can TMJ go away on its own?”
Yes, mild cases often improve with self-care within weeks. But if symptoms persist beyond 4 weeks or worsen, professional evaluation is recommended.
2. “What kind of doctor should I see for TMJ?”
Start with a dentist who has TMJ experience, or seek an orofacial pain specialist directly. Your primary care doctor can also provide referrals.
3. “How long does TMJ treatment take?”
It varies widely. Some patients improve in weeks with simple interventions; others need months of treatment. Chronic cases may require ongoing management.
4. “Is TMJ treatment covered by insurance?”
Often partially, but coverage varies. Dental insurance may cover some aspects, medical insurance others. Ask your provider about coverage before starting treatment.
5. “Will I need surgery?”
Only about 5% of TMJ patients need surgery. Most respond well to conservative treatments like physical therapy, night guards, and stress management.
6. “Can a dentist really treat TMJ?”
Some dentists have additional training in TMJ disorders. Look for one who offers comprehensive TMJ evaluation and treatment, not just night guards.
7. “How do I know if my TMJ is serious?”
See the “7 Signs” in this article – if you have any of these red flags, it’s time for professional evaluation.
8. “What if I can’t afford a TMJ specialist?”
Start with your general dentist or primary care doctor. They can often provide initial care or refer you to lower-cost options. Some dental schools offer reduced-cost TMJ treatment.
9. “Can stress really cause TMJ?”
Stress is one of the biggest contributing factors. It increases muscle tension, clenching, and grinding – all of which strain the TMJ.
10. “How do I find a good TMJ doctor?”
Look for:
- Dentists with continuing education in TMJ
- Orofacial pain specialists (board-certified)
- Physical therapists specializing in craniofacial therapy
- Ask for referrals from trusted healthcare providers
- Read reviews from other TMJ patients
Conclusion
Knowing when to see a doctor for TMJ pain isn’t always straightforward, but this guide gives you clear signposts. Mild, occasional symptoms often respond to self-care. But persistent pain, jaw locking, significant tooth damage, ear symptoms without infection, facial swelling, or declining quality of life all point to the need for professional help.
Trust your instincts. If something feels wrong with your jaw, it probably is. You don’t need to suffer in silence or wait until the problem becomes severe. Early intervention often leads to better outcomes with simpler, less invasive treatments.
The right healthcare provider can make all the difference – not just in reducing pain, but in restoring your quality of life. You deserve to eat, speak, laugh, and live without jaw pain holding you bac